This article is a review of methods for incorporating concerns for fairness or equity in economic evaluation of health care and public health programs. By way of background, the next two sections review the role of equity concerns relative to concerns for efficiency and cost-effectiveness in actual health policy on the one hand and in health economics on the other hand. Section Concerns for Equity: Overview gives an overview of a number of different kinds of concerns for equity and highlights the most salient ones. In section Methods for Incorporating Concerns for Fairness into Economic Evaluation, the various methods for incorporation of equity concerns in economic evaluation are explained.
Equity In Health Policy
Health care decision makers are interested in equity in the finance and delivery of health care, and public health decision makers are interested in equity and inequality in health more broadly. The nature and importance of these equity objectives varies between countries, reflecting variation in concerns for fairness between different societies and over time. For example, in the US policy concerns for fairness in health care focus on offering all citizens a decent minimum of health care but, beyond that, tolerating substantial inequalities of access to health care and substantial risks of catastrophic household expenditure on health care. Although in most other high-income countries policy concerns about fairness in health care focus on minimizing catastrophic household expenditure on health care, minimizing socioeconomic inequality in health care, giving priority to the worse off, and securing equal access to people with equal need. Despite this heterogeneity between different societies, important concerns for fairness exist in all societies, which health sector decision makers need to reflect in their decision making.
Fairness concerns sometimes clash with efficiency concerns. For example, health care decision makers routinely face clashes between the efficiency concern to do as much good as possible with scarce resources and the fairness concern to give priority to the most severely ill patients. Such clashes are seen, for example, in relation to dialysis machines, intensive care for preterm babies, and new drugs for end-of-life cancer patients. In each case, these forms of care are often not cost effective by conventional standards, implying that health decision makers could do more good by diverting scarce resources to other more cost effective forms of care. Yet decision makers often choose to fund these cost ineffective forms of care, reflecting important concerns for fairness that lie outside the conventional calculusof economic evaluation. Clashes of this kind are likely to become more frequent and more intense over time, even in high-income countries, as cost-increasing medical innovation increasingly drives a wedge between what is technologically possible and what publicly funded health systems can afford.
Similarly, public health decision makers in all countries routinely face clashes between improving population health and reducing socioeconomic inequality in health. For example, smoking cessation programs, physical activity programs, and other public health programs that seek to change lifestyle behavior are typically more effective in higher socioeconomic groups – and hence tend to increase socioeconomic health inequalities. Decision makers may therefore seek to redesign such programs to encourage participation among lower socioeconomic groups. In doing so, however, they may incur additional costs and limit the scope for improving health among socioeconomically advantaged populations, thus potentially reducing the sum total gain in population health. Clashes of this kind are fundamental and perennial issues in public health. The nature, size, and persistence of health inequalities are well-known. Yet policy makers still do not know how to reduce them. For example, despite a series of concerted attempts by the UK government in the 2000s to tackle health inequality, the 2010 Marmot Report found a gap of 14 years in disability-free life expectancy between the most and least deprived twentieths of small areas of England. Equity concerns of this kind are likely to become sharper over time, as global economic growth continues to be driven by technological innovation and other factors favoring high-skill workers. Applied economic evaluation evidence is needed about the costs and benefits of alternative programs for tackling health inequalities, to identify what works and to measure not only effects on average health outcomes but also effects on the socioeconomic distribution of health outcomes.
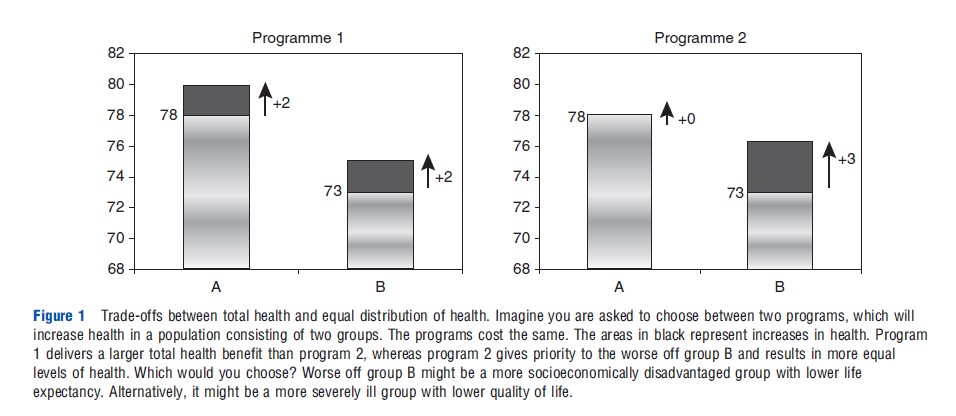
Figure 1 presents a simple stylized example of the two kinds of trade-off described above. Program 1 maximizes total health – it yields a gain of 2 health units for both groups – whereas program 2 results in a more equal distribution of health – it yields a gain of 3 health units for the worse off group B, but nothing for the better off group A. If group B is a severely ill group and the health units represent quality of life on a 0–100 scale, then this is a trade-off between total health and priority to the most severely ill patient group. If group B is a socioeconomically disadvantaged group and health units are life-years, then this is a trade-off between total health and socioeconomic inequality in life expectancy.
Equity In Health Economics
Health economists have made progress in the economic evaluation of health programs in recent decades. In the 1970s, the very idea of ‘cost-effectiveness’ was controversial among the medical community, methods were developmental, and applied economic evaluations were rarely used to inform real health care resource allocation decisions. Since then, health economists have developed sophisticated methods of economic evaluation that are now routinely used around the world to inform decisions about the funding of new health care technologies for particular groups of patients.
However, progress has focused on addressing concerns for efficiency, or cost-effectiveness, defined in terms of maximizing population health within a fixed health budget. Less attention has been devoted to addressing concerns for equity or fairness. Considerable methodological research has been done, and a variety of different theories and methods have been proposed for incorporating concerns for fairness into the economic evaluation of health programs. However, most of these methods remain developmental and even the most finished ones are still almost never used in the applied economic evaluations used to inform real resource allocation decisions.
The specific methods that have been proposed are reviewed in section Methods for Incorporating Concerns for Fairness into Economic Evaluation. Before that, it is useful to summarize the most frequently mentioned concerns for equity.
Concerns For Equity: Overview
In health care, concerns for equity often relate to the general principle that health care should be distributed in relation to need. This general principle can be divided into a vertical equity principle of greater treatment for greater need and a horizontal equity principle of equal treatment for equal need. Box 1 lists some potential concerns for fairness in health care that are often raised in relation to economic evaluations of new health care technologies. The first set of concerns, about prioritized patient subgroups, raises issues about which patients are in most ‘need’ – i.e., concerns for ‘vertical equity’. The second category is about wishes not to discriminate between patients with the same degree of ‘need’ – i.e., concerns for ‘horizontal equity’. The third set of concerns, about nonpatient benefits and nonhealth benefits, raise issues about how far ‘need’ relates to the needs of carers and dependents, as well as the needs of the patient, and how far ‘need’ relates to nonhealth needs as well as health needs. The fourth set of concerns, about industrial factors, raises issues about how far wider social policy objectives can be traded off against the equity principle of distribution according to need. The latter two categories can be thought of as concerns for efficiency, broadly construed to incorporate nonhealth benefits as well as health benefits, as opposed to concerns for fairness. However, they are important issues of social value judgment in health care resource allocation that go beyond concern for efficiency narrowly construed in the sense of health maximization.

In public health, as opposed to health care, concerns for equity often focus on reducing inequalities in population health – such as differences in life expectancy between socioeconomic groups. However, distinguishing between ‘fair’ and ‘unfair’ health inequality is problematic. Political and economic theorists have proposed numerous rival theories of what counts as ‘fair’. Key dilemmas include how far decision makers should be concerned with:
- health inequality versus priority to improving the health of the worst off;
- inequality of income and other social determinants of health versus inequality in health;
- absolute inequality (e.g., gaps) versus relative inequality (e.g., ratios);
- inequality between groups versus inequality within groups (e.g., between individuals);
- univariate health inequality (i.e., the ‘pure’ distribution of health) versus bivariate health inequality (i.e., the joint distribution between health and one unfair determinant of health, such as income) versus multivariate health inequality (i.e., the joint distribution between health and multiple unfair determinants of health);
- avoidable versus unavoidable health inequality;
- compensable versus incompensable health inequality; and
- inequality of achieved health versus inequality of opportunity for health.
Each dilemma raises difficult value-laden issues of definition and measurement (see separate entries on ‘Techniques for measuring equity in health and health care’, and ‘Field of inequality of opportunity in health’).
Methods For Incorporating Concerns For Fairness Into Economic Evaluation
The most ambitious approaches to incorporating concerns for fairness into applied economic evaluations are formal numerical value functions that take both efficiency and equity into account. The authors first review these. Less ambitious approaches include systematic characterization of relevant health equity concerns, multicriteria decision analysis, and estimation of the opportunity costs of equity. The authors return to these later on.
Formal Numerical Value Functions
In formal numerical value functions, trade-offs between efficiency and equity are expressed at a cardinal level of measurement, allowing for the overall value of an intervention or program to be estimated at that same level of measurement and thus made directly comparable with intervention or program costs. Formal value functions can in principle be applied in a fairly ‘algorithmic’ fashion, in the sense of requiring decision makers to use a single all-purpose set of social value judgments about equity, which leaves little room for deliberation and consultation with stakeholders about the appropriate set of value judgments to apply in each particular case. With suitable sensitivity analysis, however, formal value functions can also in principle be used in a more ‘deliberative’ fashion, in the sense of helping decision makers and stakeholders to deliberate their way toward a suitable set of value judgments. In this more ‘deliberative’ role, formal numerical value functions can help answer the questions: what are the implications of different value judgments for decision making in this case, and what implications might such value judgments have for other decisions in other contexts?
The Social Welfare Function
One approach is to value health programs as a mathematical function of the distribution of health among individuals or groups in the relevant population. The standard theoretical framework that economists have used is a social welfare function, which takes as its arguments individual health or group average health, which might be measured, for example, using expected lifetime quality-adjusted life-years (QALYs). The social welfare function is typically increasing in health, reflecting concern for efficiency in the sense of health maximization. However, the social welfare function need not be a simple linear sum of individual or group average health. Instead, it may give more weight to improvements in health for some individuals or groups than others, depending on societal concerns for fairness.
One social welfare function is the isoelastic or CobbDouglas function, first proposed in a health context by Adam Wagstaff and subsequently used by Paul Dolan and Aki Tsychyia and others to empirically estimate ‘equity weights’ based on surveys of public views. In the simplest case of two individuals (or groups), this function takes the following form:
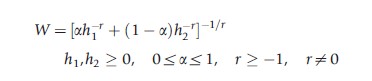
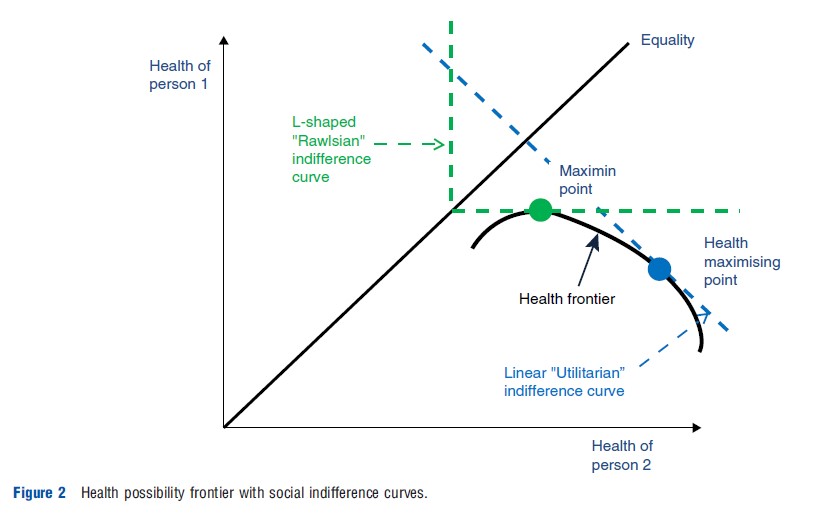
where h1 and h2 are respectively the health of person 1 and person 2 (or the average health of group 1 and group 2). This function can be visualized as a set of social indifference curves that pick out a socially preferred point on the health possibility frontier, see Figure 2. Points to the southeast of the maximin point are ‘Pareto efficient’, in the sense that the health of one person cannot be improved without reducing the health of another person. The social indifference curves pick out the best or fairest of these multiple ‘Pareto efficient’ points along the health frontier. Two parameters determine the shape of the social indifference curves. First, a general inequality aversion parameter, r, reflecting general aversion to health inequality between all individuals or groups. The magnitude of this parameter reflects the degree of curvature of the social indifference curves. Zero inequality aversion implies straight line ‘utilitarian’ style indifference curves, with r =-1, as illustrated by the blue-dashed lines, which pick out the health maximizing point in Figure 2. Complete inequality aversion implies L-shaped ‘Leontief’ or ‘Rawlsian’ style indifference curves, as r approaches infinity, as illustrated by the green-dashed lines, which pick out the maximin point in Figure 2. Second, a special priority parameter, a, reflecting priority to individuals or groups with a special equity-relevant characteristic (e.g., low socioeconomic status). This parameter would pivot the social indifference curves about the 45 degree line of equality. When additional individuals or groups are added into the analysis, additional special priority parameters can be added to allow for additional equity-relevant characteristics (e.g., ethnicity, disability, responsibility etc.), whereas the general inequality aversion parameter will apply to all individuals or groups in the analysis.
Another type of formal approach consists of weighting QALYs achieved by an intervention or program by the characteristics of the people who get the health gains, or possibly by the characteristics of the program, rather than by the resulting distribution of health. Different programs may then be compared with respect to value in terms of ‘equity-weighted QALYs’.
One approach of this kind was proposed by Alan Williams in the so-called ‘extended fair innings argument’. According to Williams, all individuals are entitled to a normal ‘fair share’ of quality-adjusted life expectancy (the ‘fair innings’). This implies that health gains to individuals below the fair innings norm – for example, the poor and disabled – should receive greater weight than health gains to individuals above the norm. In Williams’ approach, this is achieved by multiplying QALY gains by separate fair innings weights. A similar model was proposed by Han Bleichrodt and colleagues, whose ‘rankdependent utility’ theory weights individuals according to their rank in the distribution of expected lifetime health. Other approaches focusing on equality in life time health have been proposed by Magnus Johannesson and Ole Frithjof Norheim.
A problem with models that focus on equality in life time health is the implication that health gains to older individuals who have already enjoyed a long and healthy life should receive lower weight than health gains to younger individuals expected to have a shorter or less healthy life. This could, for instance, mean that pain relief in an elderly person would receive lower priority than pain relief in a young person with a life expectancy below that of the elderly person, assuming the pain relief in both cases has the same cost per QALY gained.
Another approach to equity weighting of QALYs is so-called ‘cost-value analysis’ (CVA, mentioned below). In this approach, health gains in terms of QALYs are valued more the more severe the condition of the target group is. The approach furthermore discriminates less strongly than the conventional QALY maximization approach does between gains for people with equal severity of illness with different capacities to benefit from treatment – for example, due to differences in disease, age, or comorbidity. Erik Nord and colleagues showed in 1999 that these two features may – as with concerns for fair innings – be achieved by application of separate equity weights. However, the main approach in CVA is to replace conventional utilities by ‘societal values’ that – in a coordinate diagram with utilities on the x-axis and societal values on the y-axis – form a curve that is convex toward the y-axis and compresses moderate and mild problems toward the upper end of the 0–1 scale (mentioned above).
In the Netherlands, a government guideline from 2009 indicates that willingness to spend public money in order to gain a QALY will range from 10 000 euros for conditions of little severity to 80 000 euros for conditions of great severity. This ‘graded willingness to pay’ is effectively the same as assigning severity weights to QALYs. In the Dutch context, severity is measured in terms of ‘proportional shortfall’, which builds on ‘absolute shortfall’. Absolute shortfall is the difference between a patient’s expected remaining QALYs and the number of remaining QALYs in average individuals of the same gender and age. Proportional shortfall is absolute shortfall relative to the number of remaining QALYs in average individuals of the same gender and age.
Preference Data
All the above models require data on societal preference regarding trade-offs between efficiency and equity. Only on the basis of such data can the models be of practical use.
Preference for such trade-offs are normally elicited from samples of the general population. They can be elicited in various ways.
In estimating parameters in a social welfare function, one possible approach is to ask subjects to compare different possible health scenarios for a set of social groups. The scenarios might vary, for example, with respect to average health in terms of quality-adjusted life expectancy (QALE) and the distribution of QALE between groups. Subjects may be asked to compare scenarios pairwise, and their willingness within each pair to trade-off equality for gains in average health (and vice versa) may be observed. Through statistical techniques the central tendency of such trade-offs may then be used to estimate parameters in the social welfare function. This approach has not been widely applied, but was used by Paul Dolan and Aki Tsuchyia in 2009 in a small-scale methodological study.
Another approach is the person trade-off technique as described by Nord in 1995. This is commonly used to obtain equity weights for QALYs. The basic format is that subjects are asked to compare health gains for different groups of people that differ on some variable that is considered relevant for equity reasons. For instance, subjects are asked to consider a group A of 10 people who can obtain an improvement from 0.6 to 0.8 on a 0–1 utility scale. Another group B of N people can obtain an improvement from 0.8 to 1.0. All else equal, the health gain in terms of QALYs is equally large for each individual in the two groups. But people in group A are worse off. QALYs to them may therefore be valued more highly than the same number of QALYs to people in group B. To measure the strength of preference for the more severely ill group, subjects are asked how many people there would have to be in group B for that program to be considered equally worthy of funding as the program for group A. If the mean response is 20 BB10 A, the implication is that the improvement from 0.6 to 0.8 is valued twice as highly as the improvement from 0.8 to 1.0. Weights for age and duration of benefits can be obtained in a similar fashion. In the last three decades, results from a number of person trade-off studies in different countries have been published. In principle, the results may be used as guidance in construction of models of equity-weighted QALYs. In practice, however, little use has hitherto been made of these data, partly because of uneasiness about their accuracy. An exception is Norway, where the Norwegian Medicine Agency since 2000 has recommended that conventional cost-utility analyses in terms of QALYs be supplemented by analyses using person trade-off-based health state values.
A third measurement approach was introduced by Paul Dolan in 1998. He asked subjects to compare a health gain from utility level 0.2 to 0.4 for a person A with a gain from level 0.4 to level X for a different person B. What would X have to be for subjects to consider the two health gains equally worthy of funding? On average, subjects answered 0.8, which suggests that they thought person A deserved a ‘severity weight’ of 2 compared to person B.
Finally, a fourth approach is to use pairwise choices between different groups with different health gains. This is similar to the person trade-off approach, except that individual subjects do not directly state their strength of preference but instead this is indirectly inferred from between-subject and/or within-subject patterns of pairwise choices using statistical modeling methods. This ‘stated preference’ or ‘discrete choice experiment’ approach has for instance been used in the UK by Rachel Baker and colleagues.
Other Approaches To Incorporating Concerns For Equity
Systematic Characterization Of Relevant Health Equity Concerns
This approach merely aims to foster a more systematic approach to identifying and characterizing the equity considerations at stake and to presenting relevant qualitative and quantitative background information that decision makers may find helpful. It might be useful, for instance, to develop a ‘checklist’ of potentially relevant equity concerns, based on precedent from past decisions and deliberation among stakeholder groups. Where a particular concern on the checklist is deemed relevant to the decision in hand, it would then be useful to present background information about the importance of this concern to the decision in hand. This might include qualitative information about stakeholder views and prior decision precedents; it might also include quantitative information, which puts the relevant equity concern into perspective – for instance, about how large and important the decision-relevant health inequality is compared with other health inequalities.
Multicriteria Decision Analysis
Multicriteria decision analysis aims not only to provide a qualitative ‘checklist’ of equity concerns but also to give each concern a numerical score and weight so as to arrive at an overall ranking of decision options. This approach has been advocated by Rob Baltussen and Louis Niessen in the context of both local and national health care planning in low and middle income countries, and has from time to time been used in health care priority setting exercises conducted in high-income countries. An advantage of this approach over an informal ‘checklist’ is that the scoring and weighting process can facilitate stakeholder engagement, transparency, and consistency. However, this approach does not integrate fairness concerns within economic evaluation – rather it takes the results of economic evaluation as one of many parameter inputs into a broader quantitative assessment. Furthermore, methods for the scoring and weighting of criteria currently lack the analytical rigor and evidential basis of methods for economic evaluation: much of the scoring and all of the weighting is typically done using decision maker or stakeholder opinion.
Health Opportunity Cost Of Equity
A third approach aims to estimate the health opportunity cost of a particular equity concern – for example, in terms of QALYs forgone by pursuing a more ‘equitable’ option compared with the QALY maximizing option. Every departure from health maximization on grounds of equity has an opportunity cost in terms of sum total health forgone. The size of that opportunity cost is a test of how important that equity concern is deemed to be.
This approach can be implemented using the standard methods of cost-effectiveness analysis, using the cost per QALY threshold to represent the health opportunity costs of unknown displaced programs. Or, if displaced programs can be identified and evaluated, mathematical programming can be used based on data rather than assumptions about the opportunity costs and equity characteristics of displaced program. Either way, one can compute the opportunity cost of equity by computing the difference in total net QALY benefit between ‘more efficient’ and ‘more equitable’ programs. When the equity concern relates to health inequality, this approach can be extended by calculating a health opportunity cost per unit reduction in health inequality. One could even imagine establishing a ‘cost-equality threshold’ in terms of a benchmark cost per unit reduction in health inequality from previously evaluated programs.
An advantage of the opportunity cost approach is that it can be used to address any kind of equity consideration and not just concerns about health inequality. For example, during the 1990s, the UK Standing Medical Advisory Committee advised local health authorities against adopting a racially selective policy on screening for sickle cell anemia – which is more prevalent in certain ethnic minority groups – even though this may have been the most cost-effective strategy. Franco Sassi and colleagues showed in 2001 that imposing the equity constraint of nondiscrimination imposed a health sacrifice in terms of cost-effectiveness.
A limitation of the opportunity cost approach, however, is that it only looks at the cost of the equity concern, not the benefit. It measures the equity–efficiency trade-off implied by a particular decision (a factual matter) but does not value the trade-off that policy makers ought to make (a moral matter). That is, it does not help the decision maker decide how large a sum total sacrifice (in terms of health and/or nonhealth benefits) is worth making in order to pursue a particular equity consideration. This runs the risk of lack of transparency and inconsistency across decisions, because decision makers are then free to make implicit judgments about how much health sacrifice is worth making in pursuit of a particular equity principle – and to vary those judgments from one decision to another without giving any explicit justification.
Conclusion
Health economists have developed a substantial and growing body of theoretical tools and empirical methods for incorporating concerns for fairness into economic evaluation. However, these methods have not yet been taken up and applied in routine economic evaluations used to inform resource allocation decisions. There are two main barriers to this. First, concerns for fairness are contested and context specific. Second, research requirements for measuring population preference for fairness are often greater than those for measuring health and valuations of health. Data on preference for fairness are therefore much more limited than valuation data used in estimating efficiency.
These barriers to progress are not insurmountable. As the authors have shown, there are ways of specifying equity objectives in such a way they can be quantified in economic evaluation. As pressures for transparency and accountability in public life increase, and as clashes between equity and efficiency concerns in health care and public health become ever more apparent and insistent, policy makers may be persuadable to articulate more specific health equity goals. To the extent that these equity goals are context specific, it may be possible to harness deliberative approaches to facilitate stakeholder ‘buy-in’ to particular equity goals and analytical approaches in particular decision-making contexts. Furthermore, data sources are increasingly rich as are the methods available for analyzing them. Person trade-off data already yield some useful information for equity weighting of QALYs. Methods of evidence synthesis are available for combining patient level data from a network of randomized control trials along with observational data sources. These methods could be exploited to generate information on the distribution of health effects between equity-relevant patient groups. Econometric methods are available for identifying causal effects and subgroup heterogeneity in causal effects, by exploiting observational data from surveys, administrative databases and trials – including record-linkage studies that link together all three types of data. A key challenge for the next generation of health economists is to harness these data and methods in ways that fit the contours of societal concerns for fairness and deliver analytical insights that health sector decision makers find convincing and useful.
References:
- Baltussen, R. and Niessen, L. (2006). Priority setting of health interventions: The need for multi-criteria decision analysis. Cost Effectiveness and Resource Allocation 4, 14.
- Bleichrodt, H., Diecidue, E. and Quiggin, J. (2004). Equity weights in the allocation of health care: The rank-dependent QALY Model. Journal of Health Economics 23, 157–171.
- Cookson, R., Drummond, M. and Weatherly, H. (2009). Explicit incorporation of equity considerations into economic evaluation of public health interventions. Journal of Health Politics, Policy, and Law 4, 231–245.
- Culyer A. J. and Bombard Y. (2011). An equity checklist: A framework for health technology assessments. Centre for Health Economics. CHE Research Paper 62, University of York.
- Dolan, P., Shaw, R., Tsuchiya, A. and Williams, A. (2005). QALY maximisation and people’s preference: A methodological review of the literature. Health Economics 14(2), 197–208.
- Dolan, P. and Tsuchiya, A. (2009). The social welfare function and individual responsibility: Some theoretical issues and empirical evidence. Journal of Health Economics 28, 210–220.
- Epstein, D. M., Chalabi, Z., Claxton, K. and Sculpher, M. (2007). Efficiency, equity, and budgetary policies: Informing decisions using mathematical programming. Medical Decision Making 27(2), 128–137.
- Fleurbaey, M. and Schokkaert, E. (2009). Unfair inequalities in health and health care. Journal of Health Economics 28, 73–90.
- Johannesson, M. (2001). Should we aggregate relative or absolute changes in QALYs? Health Economics 10, 573–577.
- Nord, E. (1995). The person trade-off approach to valuing health care programs. Medical Decision Making 15, 201–208.
- Nord, E., Pinto, J. L., Richardson, J., Menzel, P. and Ubel, P. (1999). Incorporating societal concerns for fairness in numerical valuations of health programmes. Health Economics 8(1), 25–39.
- Norheim, O. F. (2001). Gini impact analysis: measuring pure health inequity before and after interventions. Public Health Ethics 3(3), 282–292, doi:10.1093/phe/phq017.
- Sassi, F., Archard, L. and Le Grand, J. (2001). Equity and the economic evaluation of healthcare. Health Technology Assessment 5, 3.
- van de Wetering, E. J., Stolk, E. A., van Exel, J. A. and Brouwer, W. B. F. (2013). Balancing equity and efficiency in the Dutch basic benefits package using the principle of proportional shortfall. European Journal of Health Economics 14(1), 107–115, doi:10.1007/s10198-011-0346-7.
- Wagstaff, A. (1991). QALYs and the equity-efficiency trade-off. Journal of Health Economics 10(1), 21–41.
- Williams, A. (1997). Intergenerational equity: An exploration of the ‘fair innings’ argument. Health Economics 6(2), 117–132.