Introduction
In health insurance, cost-sharing refers to payments that a patient makes directly (i.e., out of pocket) for medical services. Cost-sharing includes a deductible, which is the amount of money a patient pays for services before their health insurance coverage begins, copayments, which are flat payments made for particular products or services (e.g., $15 for a doctor visit or $10 for a prescription), and coinsurance, which is when patients are required to pay a fixed percentage of the cost of their care (e.g., 20% of the cost of a hospital stay).
The extent that cost-sharing affects patient demand for care has long been an important topic in health economics, and research aims to answer questions about how to trade-off moral hazard and risk protection and determine optimal levels of cost-sharing. Risk protection describes protection from financial loss in the case of serious illness, and is often the reason people purchase health insurance. With more complete insurance (i.e., lower cost-sharing) consumers have better protection against losses in wealth from medical care utilization. In contrast, moral hazard in health insurance occurs when patients choose to consume care that they value less than its marginal cost because they pay little or no cost-sharing for the care. Thus, in contrast to risk protection, more complete insurance induces greater use of economically inefficient care.
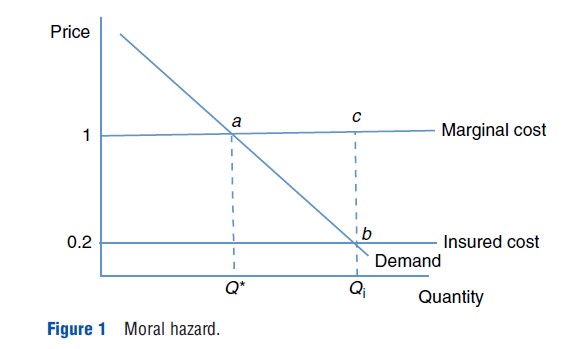
The framework that economists have traditionally used to analyze cost-sharing and to depict the inefficient use of resources due to moral hazard is illustrated in Figure 1. A demand curve (D) shows the valuation placed by the consumer on units of medical care, and the marginal cost curve represents opportunity cost, i.e., the valuation placed by consumers on those resources if used to produce other goods or services. In a competitive economy, price equals marginal cost. Each additional unit of medical care that is consumed beyond where the marginal valuation equals marginal cost (point a in Figure 1) carries with it inefficiency, because the medical care is valued less than the cost of the resources used to produce it. This deadweight loss is equal to the vertical distance between the demand curve and the marginal cost curve. It can be seen from this framework that the subsidy provided by health insurance, which reduces the consumer’s cost for medical care from marginal cost to the insured cost (here assuming a 20% coinsurance rate), induces additional resources into the production of medical care services beyond the efficient level (the insured consumer demands the amount Qi, which is greater than Q*). In Figure 1, the deadweight loss from this moral hazard is depicted by the triangle abc. Deadweight loss from moral hazard varies with price elasticity of demand: Insurance providing coverage for services that are more price elastic will induce more inefficiency than insurance coverage for services that are less price elastic.
The argument made in this welfare economics framework requires several strong assumptions, many of which likely do not hold in healthcare settings. One that is certainly violated is that patients have well-defined preference for medical care and that when they visit a doctor those preference are honored in the manner they wish. Instead, the asymmetrical information between a patient and his physician makes the agency relationship central to delivery of healthcare (e.g., patients visit their physician precisely to obtain a diagnosis and be advised on treatment) and there is considerable evidence that the way that providers are paid affects how patients are treated. Under these circumstances, an observed demand curve does not accurately reflect patient`s preference. There is also growing evidence that in complex, highstakes settings (an apt description of many healthcare settings) consumers do not make rationally consistent choices, which violates a tenant of utility maximization that is required for this framework to hold. Hurley (2000) offers a thorough discussion and critique of the traditional framework, and reviews an alternative framework, which taking a distributional approach at the societal level, suggests the focus be on utilization with an aim toward allocating resources so as to achieve equality of health across individuals. The behavioral response to cost-sharing and estimates of elasticity of demand are important to achieving optimal outcomes under this framework as well.
A Brief Review Of The RAND Health Insurance Experiment
The gold standard for evidence on the price elasticity of demand for medical care is from the RAND Health Insurance Experiment (HIE), a large-scale project that implemented a randomized study design to assess the impact of cost-sharing on demand for healthcare in the 1970s and early 1980s. The HIE randomly assigned nonelderly families to commercial insurance plans with varied coinsurance rates and deductible levels, and followed them from 3 to 5 years to study their medical care use and health. Briefly, researchers found that consumers facing higher cost-sharing consumed less care, and they estimate an elasticity of demand for medical care of 0.2 for almost all services studied, except for mental health services and dental services for which demand is estimated to be more responsive. For an average person the difference in medical care utilization did not have an adverse impact on health; individuals who were sick and had low income did experience some adverse health effects as a result of consuming less care in the higher cost-sharing plans. Aron-Dine et al. (2013) have recently reexamined this experiment and note that nonlinearities in health insurance contracts can have important effects on how consumers make decisions about their spending at different levels of budgets.
Need For More Recent Evidence
A few factors have led to continued interest in research on the price elasticity of demand for medical care following the HIE. The HIE studied the cost-sharing provisions included in insurance policies of the 1970s. At that time it was rare for a health plan to have a network of physicians or to provide coverage for prescription drugs. At present, insurers create networks of physicians and drug formularies in order to increase their negotiating power to receive more favorable prices. Physicians, physician groups, or pharmaceutical companies have an incentive to grant a lower price or a discount to be in the network or on the formulary in order to obtain a greater volume of business due to the lower patient payment for the drug or visit. For patients, physician networks and formularies has meant that cost-sharing is differential by provider or by drug, so that patients pay lower cost-sharing to see a physician who is in their plan’s network or to buy a prescription drug that is a generic or a preferred brand (i.e., on the ‘formulary’). Differential cost-sharing raises the empirical question of estimation of cross-price elasticities, which is the impact of a change in the price of one medical service on use of another medical service. If changing the price of one medical service increases (decreases) the use of another medical service, this would either add (or subtract) from the moral hazard that occurs as a result of demand for the service whose price changed.
The way health plans pay providers has also changed since the 1970s, with implications for estimates of elasticity of demand. Capitation, where plans pay providers a fixed, permember-per-month payment, has been employed by Health Maintenance Organizations (HMOs) and Preferred Provider Organizations (PPOs) over the past 20 years and is an important component of the new Accountable Care Organizations. Under this payment mechanism providers are incented to deliver less care, despite any demand by patients, because they keep the balance of their capitated payments. These incentives did not exist in the health plans that were studied under the HIE, where providers were reimbursed their full charges on a fee-for-service basis.
For the most part, the HIE also did not study use of differential cost-sharing by type of service, though one plan in the HIE varied the cost-sharing a patient would pay for inpatient versus outpatient services (i.e., cost-sharing was applied to outpatient services and inpatient services were free to the patient). The price of outpatient care was not found to affect the demand for inpatient care. However, consumers today face numerous differential prices for medical services, including across types of visits (office visits vs. emergency room visits), types of drugs (generic vs. brand), and even for some, according to the efficiency and quality of their provider through tiered provider networks. In the current environment, optimal cost-sharing depends on cross-price elasticities along with own-price elasticities.
Finally, the HIE focused on a generally healthy, commercially insured population and did not study whether demand response varied differentially for subgroups of consumers (e.g., low income/uninsured, the elderly, and racial minorities).
Thus, due in part to the evolution in benefit design and in part to the desire to test the generalizability of the HIE estimates, several studies of demand response to aspects of medical care have been conducted since the HIE. All are observational studies, the best generally consisting of natural experiments such as the introduction of new insurance policies when patients are subject to plausibly exogenous changes in cost-sharing for medical services.
Estimates Of Own-Price Elasticity Of Demand Since The HIE
Prescription Drugs
Much recent work has studied demand response for drugs in formularies, where the typical structure is either two-tiered, where the lowest cost-sharing tier contains generic drugs and the higher tier branded drugs, or more commonly, three-tiered, where the lowest cost-sharing tier contains generic drugs, the middle tier ‘preferred’ branded drugs, and the highest costsharing tier ‘nonpreferred’ branded drugs. Several papers review this literature and find that overall, increasing pharmaceutical cost-sharing results in lower utilization of prescribed drugs, i.e., own-price elasticities are negative, and in steering patients away from nonpreferred branded drugs. Gibson et al. (2005) review 30 studies from 1974 to early 2005 and report price elasticity of demand ranging from 0.1 to 0.4. In their review of 20 years of this literature (1985–2006), Goldman et al. (2007) report that for each increase in cost-sharing of 10%, prescription drug spending decreased by 2–6% (i.e., price elasticity of demand range from 0.2 to 0.6). Huskamp et al. (2003) and Goldman et al. (2007) show that these findings are consistent across classes of drugs, including medications known to be efficacious for certain chronic diseases, such as statins, angiotensin-converting-enzyme (ACE) inhibitors, antihypertensives, and antidiabetics.
Research on pharmaceutical cost-sharing among noncommercially insured populations is still emerging. The most recent work on the effect of cost-sharing for pharmaceuticals has studied demand response among the elderly following the introduction of Medicare Part D, the Medicare prescription drug benefit. A large literature has found evidence that the introduction of Part D plans has led to lower out-of-pocket spending and higher utilization of prescription drugs, suggesting negative elasticity of demand for pharmaceuticals among the elderly. Joyce et al. (2009) found this effect on demand particularly among lower-income beneficiaries. Duggan and Scott Morton (2010) estimate the effect of Part D on changes in utilization and report that their estimates suggest an own-price elasticity of 0.38 for a Medicare recipient with average prescription drug spending.
Future work should continue to study the extent to which demand response varies for population subgroups, especially vulnerable groups such as low-income populations and racial/ ethnic minorities. Some recent work by Chernew et al. (2008) compares the experience of patients living in low-income areas (based on median household income in patient’s zip code of residence) with that of patients in high-income areas, and finds that elasticity of demand for pharmaceuticals is higher for patients in low-income areas. For the most part data limitations (specifically the lack of an indicator for race or socioeconomic status in administrative claims data) have made this research difficult.
Effect Of New Health Plan Designs
The rise of managed care since the mid-1990s has meant provider payment in the form of capitation that has increased pressure on providers to curb patient utilization of care, as discussed above. Natural experiments involving the expansion of managed care provide an opportunity to study the elasticity of demand for medical care in the presence of these supplyside incentives. Chandra et al. (2010) study changes in copayments for physician office visits and prescription drugs that accompanied the transition of the elderly (retirees) to PPO and HMO plans in the early 2000s by California Public Employees’ Retirement System, and estimate that arc elasticities of demand in a managed care environment are less than 0.1, which is about half of that observed in fee-for-service plans studied in the HIE. Goldman et al. (2006) find that in the context of implementation of parity for mental health services, supply-side management techniques kept utilization levels largely unaffected by increases in the generosity of mental health coverage, a particularly interesting finding because elasticity of demand for mental healthcare was found to be twice that for other medical care in the fee-for-service environment of the HIE.
Another form of insurance design that has experienced increasing popularity since the early 2000s is high-deductible health plans, where consumers face a large deductible (e.g., $1000 for individuals and $2000 for families) before their health plan begins to cover their costs of care. Preventive services are often exempt from the deductible, and these plans may be paired with a Health Savings Account (HSA). In a large study of the HSA plans from over 700 employers (but from 1 health insurer), LoSasso et al. (2010) found that the deductible reduced medical spending by approximately 5%, and the services that were affected tended to be smaller patient-driven services.
Cross-Price Elasticities
Several studies have investigated the impact of differential cost-sharing across medical services, which is now prevalent in health insurance, on demand. In general, this literature reports trends in spending and utilization suggesting that services are substitutes (which implies that cross-price elasticity is positive) or complements (i.e., negative cross-price elasticity), but does not calculate and estimate elasticity of demand.
Pharmaceuticals And Other Medical Services
The vast majority of the studies on this topic consider the cross-price elasticity between pharmaceuticals and other medical services. Evidence is suggestive that pharmaceuticals and other medical services are substitutes. In their review, Goldman et al. (2007) summarize the evidence that increased cost-sharing is associated with adverse medical events and outcomes for patients with chronic diseases including congestive heart failure, lipid disorders, diabetes, and schizophrenia. For example, Soumerai et al. (1991, 1994) showed that limiting the number of prescriptions in a month in a Medicaid program to three saved money on drugs but led to offsetting increases elsewhere; in the case of schizophrenic patients, the increase in other spending was 17 times the savings on drugs.
Evidence suggesting similar positive cross-price elasticities has also been observed in the Medicare population following the introduction of Medicare Part D. McWilliams et al. (2011) studied spending on nonpharmaceutical medical services in a nationally representative sample of Medicare beneficiaries, and found that the introduction of Medicare Part D resulted in a significantly differential reduction in spending for beneficiaries with limited prior drug coverage (i.e., beneficiaries who had more significant decreases in out-of-pocket spending on pharmaceuticals and presumably increased their utilization and adherence) than beneficiaries with generous prior drug coverage (i.e., those who experienced less change in out-of-pocket spending). They observe the reduced spending predominantly from lower use of inpatient services and skilled nursing facility services. Likewise, in their study of California retirees, Chandra et al. (2010) find that increased cost-sharing for pharmaceuticals led to increased utilization of inpatient hospital services. Applying this finding in the opposite direction, Rosen et al. (2005) have simulated that it would save money and improve outcomes if ACE inhibitors were made available for free for elderly diabetics in Medicare. When compared with the default cost-sharing in the Medicare drug benefit, the induced increase in the use and cost of ACE inhibitors if they were free would be more than offset by other averted medical costs.
Provider Network
Early efforts (in the 1980s and mid-1990s) by health plans to organize physicians into networks were heavily driven by the provider price or the amount of the discount a provider granted the plan from their price, and simply allowed for physicians to be ‘in-network’ or ‘out-of-network.’ These network designs required patients to pay significantly more of the cost of their care if they chose to see an out-of-network physician, and to my knowledge, there is no literature estimating cross-price elasticities for in-network versus out-of-network physicians.
More recently, insurers have begun to offer ‘tiered provider networks,’ where health insurers sort providers into tiers based on cost and quality performance, and patients pay lower cost-sharing to see a provider in a higher-performing tier. In a tiered network, although the cost-sharing differential across hospitals can be significant (i.e., differential deductible or coinsurance) the cost-sharing difference across providers is usually more modest (differential office visit copay amounts on the order of $10 or $20).
Few studies have assessed consumer response to differences in cost-sharing across tiered providers (the cross-price elasticity of demand) despite the fact that health plans have been experimenting with tiered networks since the early 2000s. Two recent studies analyzed patient-level claims data and find some evidence that consumers switch to preferred providers when the price differential between preferred and nonpreferred tiers is large (i.e., on the order of hundreds of dollars). Scanlon et al. (2008) found that some workers were more likely to select a preferred hospital (preferred status based on whether the hospital met set patient safety standards) for medical visits, workers in a second union and all patients admitted for a surgical diagnosis were no more likely to choose the preferred hospitals. Rosenthal et al. (2009) analyzed patient loyalty following the narrowing of a PPO physician network that excluded 3% (48 out of 1800) of physicians from the network. The authors find that 81% of patients of affected physicians did not continue to see those physicians following their exclusion from the network, and an additional 7% of patients saw their excluded physician only one more time.
Implications For Insurance Design
An important finding from this literature is that the simple rule that insurers should offer less generous coverage for medical services with higher demand elasticity, is not necessarily ideal. First, the large body of evidence suggesting strong cross-price elasticities across medical services (i.e., that drug consumption lowers the use of other medical services) would call for more generous coverage for prescription drugs, despite the fact that their demand response is relatively elastic. In other words, some patients, especially those with certain chronic diseases, can be induced by less cost-sharing to take actions today that will reduce their future use of medical services and/or improve their future health. It thus follows that optimal cost-sharing could vary across persons and across specific medical goods and services. This logic underlies value-based insurance design (VBID), a mechanism proposed by Chernew et al. (2007) where copayments for high-benefit services, such as medications for treatment of chronic disease, would be kept low or set to zero. Although early experience with VBID has shown promise, Baicker and Goldman (2011) offer a thoughtful discussion of the challenges of how to design the benefit design beyond pharmaceutical coverage for individuals with chronic illness, and how to address the potential for risk segmentation of patients into plans with this design.
Final Comments
The empirical research conducted since the 1970s reports estimates of own-price elasticities that are largely in line with those from the RAND HIE. Demand response for pharmaceuticals is also found to be slightly more responsive than that for other services. There is some preliminary evidence suggesting that the most vulnerable populations are more responsive to out-of-pocket medical spending; however, this question should be tested further.
In the context of managed care, cost-sharing is not the only tool to curb inefficient use of medical services. Along with capitation, insurers can apply tools such as gatekeeping and utilization review to affect consumption of medical services. Supply-side mechanisms may affect the estimates of demand response and limit the generalizability of these findings because the effect of the supply-side policies may not be known. However, that physicians have been found to treat their patients in a consistent pattern, such that patterns of care induced by managed care supply-side incentives spillover to a physician’s entire patient panel, might limit concerns about generalizability.
There is currently still much more to learn. Efforts to estimate elasticity of demand for medical services for uninsured populations is now possible due to currently ongoing natural randomized experiment among a Medicaid eligible population in Oregon (Finkelstein et al., 2012); this evidence, not yet available, will greatly enrich the literature. Several opportunities for future research in this area remain. One potential vein is to study how to incorporate findings from behavioral economics, which indicate that consumer decision-making is subject to heuristics and biases, to improve the effect of lowered cost-sharing on consumer demand and the implementation of VBID. Improving our understanding of how cost-sharing can lead to overall cost savings or encourage demand for high quality, effective medical care is an exciting future research agenda.
Bibliography:
- Aron-Dine, A., Einav, L. and Finkelstein, A. (2013). The RAND health insurance experiment, three decades later. Journal of Economic Perspectives 27(1), 197–222.
- Baicker, K. and Goldman, D. (2011). Patient cost sharing and health care spending growth. Journal of Economic Perspectives 25(2), 47–68.
- Chandra, A., Gruber, J. and McKnight, R. (2010). Patient cost-sharing and hospitalization offsets in the elderly. American Economic Review 100(1), 193–213.
- Chernew, M. E., Gibson, T. B., Yu-Isenberg, K., et al. (2008). Effects of increased patient cost-sharing on socioeconomic disparities in health care. Journal of General Internal Medicine 23(8), 1131–1136.
- Chernew, M. E., Rosen, A. B. and Fendrick, A. M. (2007). Value-based insurance design. Health Affairs 26(2), w195–w203.
- Duggan, M. and Scott Morton, F. (2010). The effect of Medicare Part D on pharmaceutical prices and utilization. American Economic Review 100(1), 590–607.
- Finkelstein, A., Taubman, S., Wright, B., et al. (2012). The Oregon health insurance experiment: Evidence from the first year. The Quarterly Journal of Economics 127(3), 1057–1106.
- Gibson, T. B., Ozminkowski, R. J. and Goetzel, R. Z. (2005). The effects of prescription drug cost sharing: A review of the evidence. American Journal of Managed Care 11(11), 730–740.
- Goldman, D. P., Joyce, G. F. and Zheng, Y. (2007). Prescription drug cost sharing: Associations with medication and medical utilization and spending and health. Journal of the American Medical Association 298(1), 61–69.
- Goldman, H. H., Frank, R. G., Burnam, M. A., et al. (2006). Behavioral health insurance parity for federal employees. New England Journal of Medicine 354(13), 1378–1386.
- Hurley, J. (2000). An overview of the normative economics of the health sector. In Culyer, A. J. and Newhouse, J. P. (eds.) Handbook of health economics, vol. 1A. Amsterdam: Elsevier.
- Huskamp, H. A., Deverka, P. A., Epstein, A. M., et al. (2003). The effect of incentive-based formularies on prescription-drug utilization and spending. New England Journal of Medicine 349(23), 2224–2232.
- Joyce, G. F., Goldman, D. P., Vogt, W. B., Sun, E. and Jena, A. B. (2009). Medicare Part D after two years. American Journal of Managed Care 15(8), 536–544.
- LoSasso, A. T., Shah, M. and Frogner, B. K. (2010). Health savings accounts and health care spending. Health Services Research 45(4), 1041–1060.
- McWilliams, J. M., Zaslavsky, A. M. and Huskamp, H. A. (2011). Implementation of medicare Part D and nondrug medical spending for elderly adults with limited prior drug coverage. Journal of the American Medical Association 306(4), 402–409.
- Rosen, A. B., Hamel, M. B., Weinstein, M. C., et al. (2005). Cost-effectiveness of full medicare coverage of angiotensin-converting enzyme inhibitors for beneficiaries with diabetes. Annals of Internal Medicine 143(2), 89–99.
- Rosenthal, M. B., Li, Z. and Milstein, A. (2009). Do patients continue to see physicians who are removed from a PPO network? American Journal of Managed Care 15(10), 713–719.
- Scanlon, D. P., Lindrooth, R. C. and Christianson, J. B. (2008). Steering patients to safer hospitals? The effect of a tiered hospital network on hospital admissions. Health Services Research 43(5p2), 1849–1868.
- Soumerai, S. B., McLaughlin, T. J., Ross-Degnan, D., Casteris, C. S. and Bollini, P. (1994). Effects of limiting medicaid drug-reimbursement benefits on the use of psychotropic agents and acute mental health services by patients with schizophrenia. New England Journal of Medicine 331(10), 650.
- Soumerai, S. B., Ross-Degnan, D., Avorn, J., McLaughlin, T. J. and Choodnovskiy, I. (1991). Effects of medicaid drug-payment limits on admission to hospitals and nursing homes. The New England Journal of Medicine 325(15), 1072.
- Ketchum, J. D. and Simon, K. I. (2008). Medicare Part D’s effects on elderly patients’ drug costs and utilization. American Journal of Managed Care 14(supplement 11), SP14–SP22.
- McGuire, T. G. (2012). Demand for health insurance. In Pauly, M. V., McGuire, T. G. and Barros, P. P. (eds.) Handbook of health economics, vol. 2. North Holland: Elsevier.
- Newhouse, J.-P. and The insurance experiment group (1993). Free for all? Lessons from the RAND health insurance experiment. Cambridge: Harvard University Press.
- Pauly, M. V. (1968). The economics of moral hazard: Comment. American Economic Review 58(3), 531–537.
- Remler, D. and Greene, J. (2009). Cost-sharing: A blunt instrument. Annual Review of Public Health 30, 293–311.
- Yin, W., Basu, A., Zhang, J. X., et al. (2008). The effect of medicare Part D prescription benefit on drug utilization and expenditures. Annals of Internal Medicine 148(3), 169–177.
- Zeckhauser, R. J. (1970). Medical insurance: A case study of the tradeoff between risk spreading and appropriate incentives. Journal of Economic Theory 2(1), 10–26.